Staphylococcus aureus. You may have had it in connection with a wound infection. In most cases, it will pass without treatment, while severe cases may require antibiotics, which kills the bacteria. This is the case for the majority of the population. In fact, many of us—though we feel perfectly fine—carry staphylococci in the nose, a good, moist environment in which the bacteria thrive.
However, more and more staphylococci are becoming resistant to antibiotics (also known as multi resistant Staphylococcus aureus or MRSA), and these infections can be difficult to treat.
“Antibiotics resistance is an increasing problem, especially on a global scale. And when you have this relatively simple infection which suddenly cannot be treated with antibiotics, the situation can turn serious, sometimes life-threatening,” says Professor Niels Ødum from the LEO Foundation Skin Immunology Research Center at the University of Copenhagen.
Therefore, all over the world, a lot of resources are being invested in fighting antibiotics resistance in Staphylococcus aureus infections, and a new study among skin lymphoma patients has produced positive results. A new substance called endolysins has proven capable of killing both resistant and non-resistant Staphylococcus aureus—without the need for antibiotics. But we will get back to that.
The discovery is good news to patients with a weak immune system to whom a Staphylococcus aureus infection can be serious and, at worst, fatal. But it also adds to the knowledge we have of other forms of treatment.
“To people who are severely ill with e.g. skin lymphoma, staphylococci can be a huge, sometimes insoluble problem, as many are infected with a type of Staphylococcus aureus that is resistant to antibiotics,” says Niels Ødum.
“That is why we are careful not to give antibiotics to everyone, because we do not want to have to deal with more resistant bacteria. Therefore, it is important that we find new ways of treating—and not the least to prevent—these infections.”
New substance may be the answer
In some patients, Staphylococcus aureus will cause the cancer to worsen. And even though antibiotics appear to work in some cases, it is not without its problems.
“We can tell that giving high doses of antibiotics to patients with serious infections causes their health, skin and cancer symptoms to improve. But once we stop giving them antibiotics, the symptoms and staphylococci quickly return. Patients experience many adverse effects, and some risk getting resistant bacteria,” says Niels Ødum.
Therefore, treating Staphylococcus aureus can be tricky. At worst, cancer patients may die of an infection which doctors are unable to treat.
And this is where endolysins enter the scene, as this new substance may be part of the solution to antibiotics resistance like MRSA.
“This particular endolysin is a brand new, artificially produced enzyme that has been improved several times and designed as a new drug,” explains Postdoc Emil Pallesen, who is first author of the study. “The great thing about this enzyme is that it has been designed to penetrate the wall of Staphylococcus aureus. This enables it to target and kill the harmful Staphylococcus and leave harmless skin bacteria unharmed.”
And that is what made the researchers decide to test the new substance; they expected it to be able to kill both resistant and non-resistant Staphylococcus bacteria.
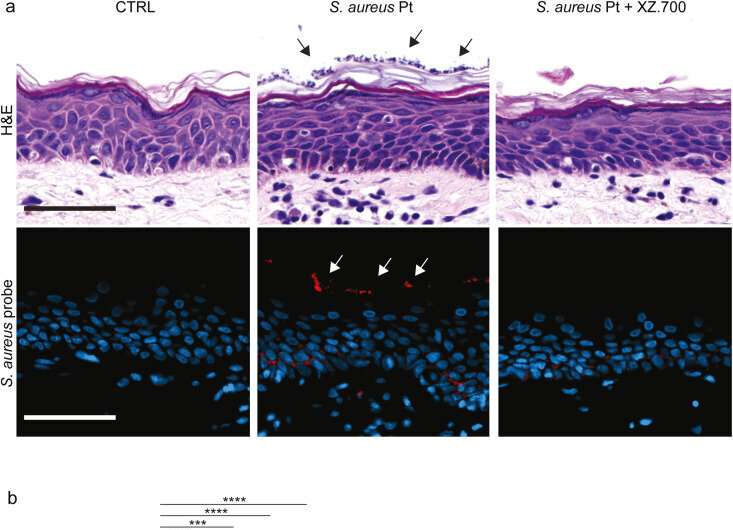
“We have been testing the substance on skin samples from patients, and it does appear to kill Staphylococcus aureus from patients. Endolysins do not care whether the bacterium is resistant to antibiotics or not, because it does not work in the same way as antibiotics,” says Niels Ødum. “The really good news is that our lab tests have showed that endolysins do not just eradicate Staphylococcus aureus; they also inhibit their ability to promote cancer growth.”
The findings are published in the Journal of Investigative Dermatology.
More information:
Emil M.H. Pallesen et al, Endolysin inhibits skin colonization by patient-derived Staphylococcus aureus and malignant T cell activation in cutaneous T cell lymphoma, Journal of Investigative Dermatology (2023). DOI: 10.1016/j.jid.2023.01.039
Journal information:
Journal of Investigative Dermatology
Source: Read Full Article