COVID-19 is an infectious disease caused by the SARS-CoV-2 virus. The main symptoms of COVID-19 resemble that of a respiratory ‘flu— ‘like disease, though symptoms vary considerably between affected individuals.
.jpg)
Image Credit: iunewind/Shutterstock.com
What is COVID-19?
Coronavirus Disease 2019, or COVID-19, is an infectious acute respiratory disease caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Initially identified in Wuhan, China, COVID-19 rapidly became a global pandemic as of 30th January 2020 and is still ongoing.
Worldwide, around 8 million cases of COVID-19 have been confirmed with around 450,000 deaths (as of June 2020).
Main Symptoms of COVID-19*
According to the NHS (UK), the 3 main symptoms of COVID-19 are:
- Fever – a high temperature >37.8OC/100OF (~86-88% of reported cases)
- Dry Cough – a new continuous cough that occurs regularly throughout the day (at least 3 coughing episodes per 24 hours) (~69%)
- Smell and Taste – a noticeable new loss in the sense of smell and taste (variable estimates – data still emerging)
However, not all affected individuals may display all 3 of these symptoms. Often, 1 of the 3 symptoms may be sufficient. Furthermore, according to the CDC (US), additional symptoms may include 1 or more of the following symptoms, which may occur in a subset of affected individuals:
- Shortness of breath or difficulty breathing (~22%) – depends on the severity of disease i.e. in more severe disease this is very common
- Fatigue (tiredness) (~35-39%)
- Muscle and body aches (~16-36%)
- Headache (~12%)
- Sore throat (~12%)
- Nausea or vomiting (~4-6%)
- Diarrhea (~5%)
- Congested or runny nose (~3%)
Many of these symptoms are also the same for influenza (flu) and cold. The main distinction between flu and COVID-19 is that flu symptoms usually begin abruptly within 1-4 days whereas COVID-19 symptoms develop gradually over 2-14 days.
Symptoms such as a runny or congested nose, in addition to body aches and pains, are more common in flu than in COVID-19.
The symptoms of COVID-19 typically disappear within 14 days after initial symptoms, and this is the basis of self-isolation, or quarantine, as imposed by many nations to combat local epidemics.
Although for the vast majority of people, symptoms disappear within 14 days, there may be some cases where symptoms do not disappear and worsen that may require hospitalization.
*Note – as COVID-19 is a new disease and the global pandemic is still ongoing, the exact symptomatic statistics may change as more evidence emerges. Furthermore, more symptoms may be added to the list in the coming months.
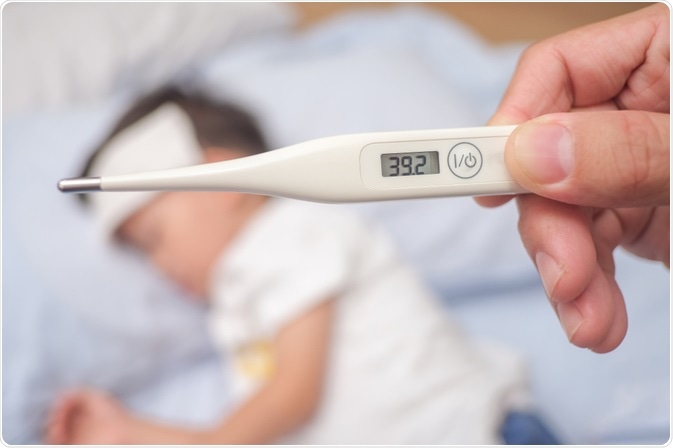
Image Credit: Yaoinlove/Shutterstock.com
Symptoms Severity
In a majority of affected individuals (80%), COVID-19 symptoms may totally asymptomatic (no obvious symptoms), very mild (barely noticeable) or mild-moderate (noticeable and somewhat affects daily living, but manageable).
In a small minority of affected individuals (5-15%), more serious and severe symptoms may occur (moderate pneumonia). Typically, these occur in older patients (over 70) and those with pre-existing chronic health conditions.
Severe disease can occur in around 10-15% of affected individuals that results in severe pneumonia, dyspnea (severe shortness of breath), tachypnea (less than 30 breaths/min), and blood oxygen saturation (SpO2) <93% on air.
This requires hospitalization, and many patients will successfully recover, with only a small minority succumbing to their condition (~2-5%). The case-fatality rate (CFR) for COVID-19 is thought to be around 5% on average, though regional variations vary from less than 1% (e.g. Singapore) – 14% (e.g. UK).
Critical disease can occur in less than 5% of all cases resulting in acute respiratory distress syndrome (ARDS) characterized by respiratory failure, septic shock (2%), multiple organ dysfunction and/or failure (1-2%).
However, the severe and critical cases account for only a small minority of all cases, and typically in those that over 70 years of age, and those with pre-existing chronic cardiovascular and respiratory health conditions.
The most common health conditions that lead to more pronounced symptoms include hypertension, diabetes mellitus, coronary heart disease, liver disease, cerebrovascular disease, COPD, cancer, renal (kidney) disease, and immunodeficiency.
Furthermore, males are affected more than females, as well as Black and South Asian ethnic minorities. Vitamin D deficiency may also be a critical factor in determining symptom (disease) severity.
It is important to note, however, some (small percentage of) younger healthier individuals may also display more severe symptoms and require hospitalization, despite no underlying conditions. Having a health condition is not necessarily a prerequisite for more severe symptoms as many with health conditions that have COVID-19 only display mild symptoms.
Paediatric Inflammatory Multisystem Syndrome Temporally Associated with SARS-CoV-2 (PIMS-TS)
Kawasaki disease is a rare disease that affects children under the age of 5 primarily and is characterized by a fever that can last around 5 days alongside a bodily rash, swollen glands, red fingers & toes, and red eyes.
The exact cause is unknown, and the disease lasts for around 3 weeks in total. Kawasaki is not transmissible and can be treated effectively using aspiring and immunoglobulin therapy. If left untreated, Kawasaki disease leads to coronary artery aneurysms in 25% of all cases. If this occurs, more advanced treatment and surgery are required. Death occurs in around 1% of those affected.
As of April 2020, many doctors and scientists noticed the emergence of a Kawasaki disease-like syndrome developing in young children where there was a high prevalence of COVID-19 – including the UK and Italy.
Although it is very similar to Kawasaki disease, it is thought to be a new disease called PIMS-TS. Researchers from Imperial College London identified over 200 cases in the UK, with most children recovered. However, if left untreated, it can be potentially very serious. It is important to state that COVID-19 is very mild & benign with extremely limited fatalities in children.
The major difference between PIMS-TS and Kawasaki disease is that PIMS-TS tends to affect older children (around 9 years of age) compared to 4-5 years. Furthermore, other key symptoms include adnominal pain and diarrhea. Another key difference is that blood test results show a higher level of inflammatory markers and cardiac enzymes suggesting enhanced cardiac strain.
Whether COVID-19 directly causes PIMS-TS or not is still unclear, however, 45/58 children in the study (published in JAMA) had evidence of current or past COVID-19 infection – and evidence suggests that PIMS-TS develops after COVID-19 infection in a very small subset of children.
It is thought that an overactive immune response to COVID-19 leads to PIMS-TS. A cytokine storm is seen in many patients with COVID-19 with more severe symptoms, thus those children with a larger immune overreaction may be susceptible.
In summary, the symptoms of COVID-19 resemble that of a respiratory ‘flu’-like disease with the main symptoms being fever, new continuous cough, and the loss of smell/taste, in addition to some degree of difficulty breathing and fatigue. Symptoms can vary considerably in strength – from totally asymptomatic through to critical respiratory distress.
Thankfully, in the vast majority of cases, symptoms tend to be mild or moderate at worst, with less than 5% developing critical symptoms. Those that develop more severe symptoms tend to be older and have pre-existing chronic health conditions.
In addition, in some young children, an inflammatory Kawasaki disease-like syndrome (PIMS-TS) can develop that requires medical attention.
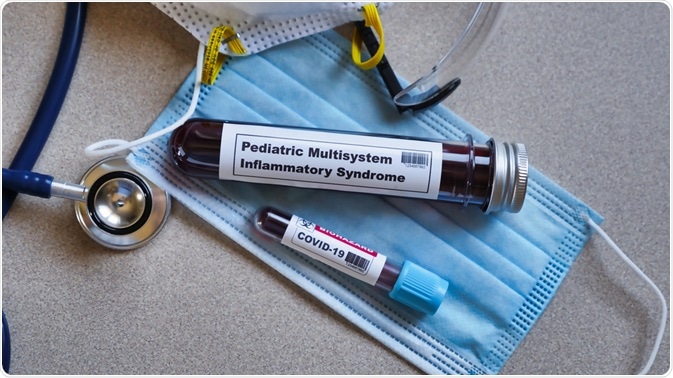
Image Credit: Bernard Chantal/Shutterstock.com
Sources:
- NHS.uk, 2020. Coronavirus (COVID-19) – Main Symptoms. https://www.nhs.uk/conditions/coronavirus-covid-19/symptoms/
- CDC.gov, 2020. Coronavirus Disease 2019 0 Symptoms. www.cdc.gov/coronavirus/2019-ncov/symptoms-testing/symptoms.html
- Cascella et al, 2020. Features, Evaluation, and Treatment Coronavirus (COVID-19). StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK554776/
- Li et al, 2020. COVID‐19 patients' clinical characteristics, discharge rate, and fatality rate of meta‐analysis. J Med Virol. 10.1002/jmv.25757 (ahead of print) https://pubmed.ncbi.nlm.nih.gov/32162702/
- Lovato et al, 2020. Clinical Presentation of COVID-19: A Systematic Review Focusing on Upper Airway Symptoms. Ear Nose Throat J. 145561320920762 (ahead of print) https://pubmed.ncbi.nlm.nih.gov/32283980/
- Whittaker et al, 2020. Clinical Characteristics of 58 Children With a Pediatric Inflammatory Multisystem Syndrome Temporally Associated With SARS-CoV-2. JAMA e2010369 (ahead of print). https://pubmed.ncbi.nlm.nih.gov/32511692/
- NHS.uk, 2020. Kawasaki Disease. https://www.nhs.uk/conditions/kawasaki-disease/
Further Reading
- All Coronavirus Disease COVID-19 Content
- What Mutations of SARS-CoV-2 are Causing Concern?
- What is the Clinical Impact of COVID-19 on Cancer Patients?
- Can Pets Get COVID-19?
- An Overview of the SARS-CoV-2 Vaccines
Last Updated: Jun 22, 2020

Written by
Osman Shabir
Osman is a Neuroscience PhD Research Student at the University of Sheffield studying the impact of cardiovascular disease and Alzheimer's disease on neurovascular coupling using pre-clinical models and neuroimaging techniques.
Source: Read Full Article